Post-Operation Therapy After Knee Replacement: The Complete Recovery Timeline
Introduction: Setting the Stage for a Successful Recovery
Undergoing a total knee replacement is a major medical milestone that marks the beginning of a transformative journey. Many patients have lived with constant, debilitating knee pain caused by osteoarthritis or injury for years, which significantly limits their movement and lowers their overall quality of life. While the surgical procedure successfully repairs the structural integrity of the knee joint, the surgery itself is merely the foundation. The true restoration of your independence relies heavily on the work you perform during the subsequent weeks and months. This guide provides a full plan for rehabilitation, framing recovery not as a simple, passive event, but as a committed partnership between you and your healthcare team to ensure a full recovery.
Why Physical Therapy is Non-Negotiable After Total Knee Arthroplasty
Physical therapy is the essential cornerstone of your recovery following knee replacement surgery. While the surgeon corrects the damage inside the knee, it is the therapist who teaches the soft tissues and muscles how to adapt to the new mechanics of your prosthetic knee. If you minimize these sessions, the risk of developing stiffness, scar tissue adhesions, or persistent muscular weakness increases dramatically.
Your physical therapist acts like a coach and guide. They adjust exercises based on your progress, manage the "good pain" from movement, and ensure that you do not push too hard in ways that could harm your healing. Through a structured home exercise program, your therapist will help you maximize your muscle strength and achieve the best possible knee motion.
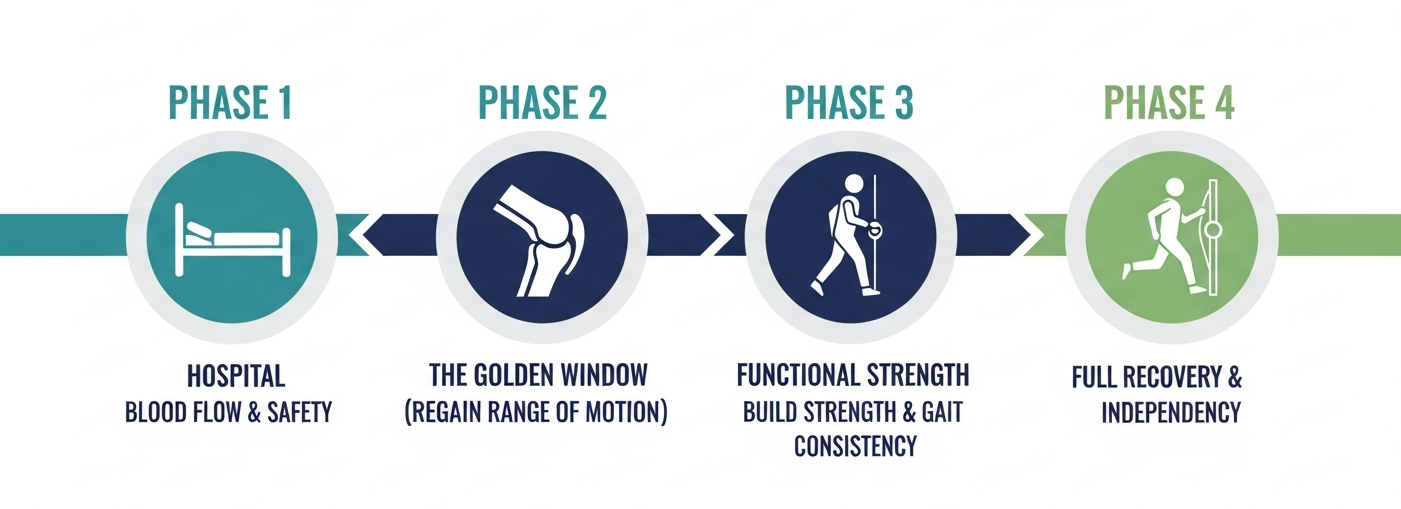
The four distinct phases of knee replacement recovery, from immediate post-operative safety to full restoration of mobility at the one-year mark.
Recovery after a total knee replacement usually follows a general path, but each person's progress is different. The process typically spans four phases, starting in the hospital where the focus is on blood flow and safety. It then moves into the "Golden Window" of the first six weeks, where regaining range of motion is the primary objective. Following this, you progress into a phase of building functional strength and gait consistency, eventually reaching the one-year mark. Understanding these phases helps you celebrate the small, essential wins that lead to long-term success.
Preparing Your Environment: The "Safety First" Home Setup
The transition from the hospital back to your personal environment is a critical phase. Creating a supportive space minimizes the risk of falls and reduces unnecessary physical strain, allowing you to focus your energy on the exercise regime prescribed by your professional rehabilitation staff.
Lifestyle Ergonomics: Modifying Your Space for Limited Mobility
Before your knee surgery, assess your living areas for hazards. Remove loose rugs, clear electrical cords from walkways, and ensure that high-traffic areas are well-lit. If your primary living space involves stairs, consider moving a temporary bed or recliner to the ground floor for the first week. Place frequently used items—such as your phone, remote, and chargers—at waist height to avoid unnecessary bending.
The Caregiver’s Checklist: How a Support Person Enhances Recovery
Having a support system is invaluable. A friend or family member can give you psychological support, which helps you handle the frustration that comes with recovery. Your caregiver should assist with medication schedules, wound monitoring, and meal prep. Ensure they understand your physical limitations and know how to assist with your walking aids.
Essential Equipment: Walkers, Canes, and Assistive Devices
You will likely be discharged with a walker for stability. Using an assistive device for a few more days is safer than rushing. Trying to walk alone before your quadriceps are ready can cause problems, such as an altered gait pattern, which is hard to fix later. Your therapist will eventually guide your transition to a cane as your confidence grows.
Phase 1: The Hospital Stay and Immediate Post-Op (Days 0–3)
Doctors watch you closely right after surgery to ensure you are stable and mobile enough to function safely in your home environment.
Waking Up from Anesthesia: Initial Sensation and Pain Management
Upon waking, you will experience soreness. Modern pain management, often involving a regional nerve block or a blood thinner to prevent a blood clot, is vital. Effective pain control enables you to engage in early physical therapy, which is essential for preventing the joint from stiffening.
Preventing Blood Clot Formation: Ankle Pumps and Compression Stockings
A primary clinical concern is the prevention of blood clot formation. You will be encouraged to perform ankle pumps—flexing and extending your feet—immediately upon waking. Combined with compression stockings or sequential compression devices, these muscle pumping exercises facilitate healthy circulation and reduce the risk of a blood clot.
Your First Steps: Standing and Walking in the Hospital Corridor
Movement is medicine. Within hours of surgery, you will stand with the assistance of a physical therapist to walk a short distance in the hospital corridor. This initial mobilization demonstrates that the new joint is stable and that you can perform basic safety tasks, such as getting in and out of a chair.
Understanding Passive vs. Active Exercises in Early Rehab
During the first few days, your therapy will focus on both passive exercises—where the therapist moves your leg—and active exercises, where you begin to fire the muscles yourself. This balance is crucial for preserving your surgical results.
Phase 2: The First Two Weeks at Home (Early Healing)
The first two weeks represent the most intense period of swelling management and functional recovery.
Managing Post-Operative Swelling: Ice Packs vs. Cryotherapy Devices
Post-operative swelling is the primary enemy of range of motion. Using an ice pack, frozen gel pack, or a professional cold compression therapy device for 20 minutes every hour is standard protocol. Elevating the leg above heart level further aids in fluid reduction.
Wound Care and Monitoring: Staples, Skin Glue, and Signs of Infection
Whether you have staples or skin glue, follow your surgeon's instructions. Watch closely for signs of infection, such as increasing redness or drainage, and report these to your medical team immediately.
Essential Exercises: Quadriceps Sets, Heel Slides, and Straight Leg Raises
Your home program will focus on firing the quadriceps. Quadriceps sets (tightening the thigh muscle) are the building blocks of stability. Heel slides help improve flexion, while straight leg raises focus on restoring the strength needed for a normal gait.
The Biomechanical Goal: Achieving Full Extension Early
Achieving full extension—getting the knee perfectly straight—is the most critical biomechanical goal in the first two weeks. A knee that does not extend fully will cause a persistent limp.
Phase 3: Weeks 3–6 (Restoring Range of Motion and Gait)
As you settle into your routine, the focus shifts toward more aggressive mobility and strengthening.
Milestone Markers: Aiming for 90-Degree Knee Flexion
By the end of the sixth week, the goal is typically to achieve at least 90 degrees of flexion. This allows you to sit comfortably and navigate stairs efficiently.
Transitioning Walking Aids: Moving from a Walker to a Cane
You will transition from a walker to a cane, and eventually to independent walking. This shift should be dictated by your gait quality.
Stationary Bicycle Training: Using a Recumbent Bike for Joint Fluidity
Using a recumbent bike is the gold standard for restoring range of motion. It allows for gentle, repetitive motion that improves joint fluidity without the impact of traditional walking.
Identifying and Managing Scar Tissue Adhesions
Scar tissue is a natural part of healing, but excessive formation can cause stiffness. Your therapist will use manual scar mobilization to prevent the tissue from binding down and restricting movement.
Phase 4: Weeks 7–12 (Strength, Stability, and Endurance)
Now that the initial surgical healing is complete, you will focus on building the stamina needed for daily life.
Advanced Muscle Strengthening: Focusing on Glutes, Hamstrings, and Calves
The entire kinetic chain is involved in walking. Strengthening your hip abductors and calf muscles reduces the stress placed on your new knee.
Gait Training: Correcting Your Walking Pattern for Long-Term Joint Health
Many patients develop a compensatory limp due to pre-operative pain. You must consciously train your brain and body to walk with a normal heel-to-toe pattern to avoid hip or back issues.
Functional Milestones: Negotiating Stairs and Driving
By this stage, most patients are safely driving and performing stair climbing. Always seek approval from your surgeon before returning to the road.
Introduction to Outpatient Therapy and Higher-Intensity Training
Outpatient therapy sessions will get harder. They will include balance training, agility, and stronger resistance exercises. These prepare you for daily life demands.
The "Plateau" and Beyond: Recovery from 3 Months to 1 Year
At the three-month mark, it is common to feel a sense of stagnation. This "plateau" is where rapid gains in range of motion level off. This is a normal part of the physiological maturation of the tissue.
Navigating the Mental Fatigue of Long-Term Rehabilitation
The recovery process is mentally taxing. If you feel your progress has halted, speak with your therapist about functional goals, such as playing with grandchildren, which is often a better metric than a few degrees of flexion.
Conclusion
A successful recovery from total knee replacement requires consistency, patience, and commitment to rehabilitation. From hospital days to the one-year strengthening phase, each step ensures your new joint's function and longevity. Prioritize physical therapy, follow safety rules, and manage physical and emotional challenges to improve your quality of life. Keep open communication with your surgeon and therapist, your key partners in this process. Your new knee can last years if you care for it properly during this crucial time. Stay disciplined, celebrate small wins, and focus on the long-term freedom of restored mobility.