Back Spasm Remedies: 7 Proven Ways to Get Fast Relief at Home
The sharp, sudden onset of Back Spasms can turn a simple morning routine into a debilitating ordeal. When your back muscles lock up, the resulting back pain often feels like a protective mechanism gone rogue. It is normal to fear movement when your spine feels weak. However, recovery needs a focused plan. This plan calms the nervous system and restores muscle function, allowing you to regain mobility and move past the discomfort of an acute injury. By understanding the mechanics of your lumbar spine, you can transition from reactive pain management to proactive healing.
What is a Muscle Spasm? (The Involuntary Contraction)
A muscle spasm is an involuntary, forceful contraction of the fibers that fails to relax. When this occurs, it creates a rigid "splinting" effect around the spinal cord. Your body is essentially trying to protect deeper structures—such as your discs, soft tissues, or vertebrae—by locking the surrounding muscles into place. While this is a physiological defense, it creates a feedback loop of pain. Distinguishing between superficial muscles and deep, intrinsic muscles is key; often, the superficial "erector" muscles seize to compensate for deeper instability caused by nerve irritation or disc herniation.
Common Triggers: From Dehydration to Muscle Strain
The triggers for muscle spasms are often cumulative. Poor posture, especially while sitting, creates chronic tension in the lower back. Furthermore, dehydration significantly impairs function; electrolytes are required for the chemical signaling that allows fibers to relax. Dehydration also makes your nervous system more sensitive, causing your muscles to overreact to small stresses. Whether it is heavy lifting, repetitive bending, or muscle fatigue, your body’s inability to maintain homeostasis often leads to this painful state.
Thermal Therapy: The Strategic Use of Ice and Heat
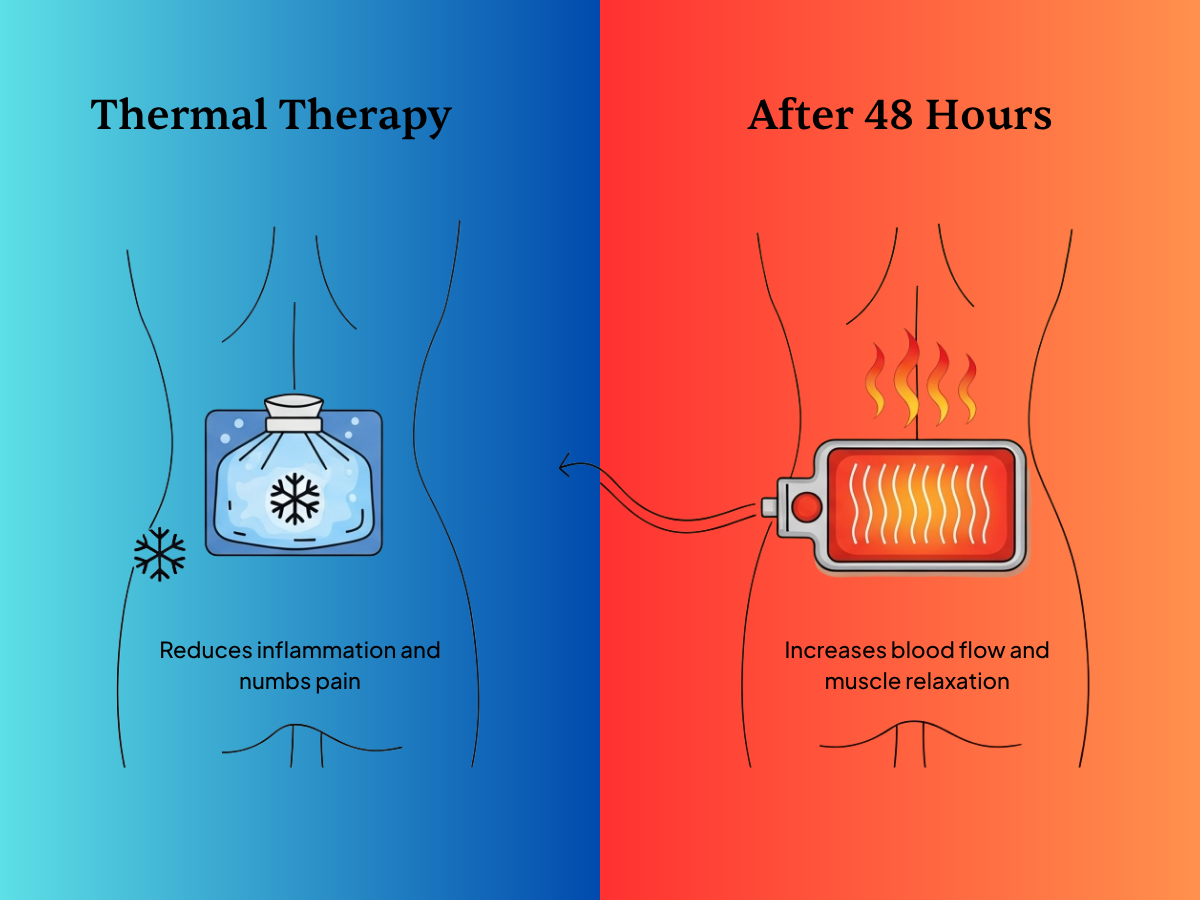
The 48-Hour Rule: When to use ice versus heat for back spasm relief.
How to Relieve Back Spasms with Thermal Therapy, Movement, and Breathwork.
You can manage inflammation with thermal therapy, while gentle movement helps hydrate the discs. Breathwork calms your nervous system, helping you control your body's protective responses.
The First 48 Hours: Using Ice Packs to Calm Inflammation
In the immediate aftermath of a spasm, inflammation is the primary enemy. Applying an ice pack for 15–20 minutes serves as a localized anesthetic, slowing nerve conduction velocity and dulling acute pain. Ice reduces the chemical response to tissue injury, helping to settle the area. Always wrap the ice in a thin towel to protect your skin.
The Recovery Phase: Applying Heat to Relax Tight Fibers
After 48 hours, heat becomes your primary tool. Heat increases blood flow, facilitating the delivery of oxygen and nutrients while flushing out metabolic waste. A heating pad helps the tightened fibers lengthen and relax, effectively breaking the physical "cramp" holding your spine in an awkward position.
The Contrast Method: Alternating Ice and Heat for Maximum Circulation
For persistent spasms, the contrast method is highly effective. By alternating between ice and heat, you create a "pump" effect in the local vascular system. This rhythmic cycle encourages fresh blood to enter the area, accelerating recovery.
Why Movement is Medicine (Avoiding the "Bed Rest Trap")
One of the most common mistakes is retreating to bed for days. The "bed rest trap" is counterproductive; inactivity leads to stiffened joints and deconditioned muscles. Your spine requires gentle, rhythmic motion to circulate synovial fluid and keep the discs hydrated. Movement is medicine when kept within a pain-free, controlled range.
The Child’s Pose: Creating Space in the Lumbar Spine
The Child’s Pose is a foundational movement for lower back relief. By kneeling and reaching your arms forward, you gently lengthen the spinal column, relieving pressure on the vertebral joints without requiring active engagement.
Knee-to-Chest: Relieving Pressure on the Vertebrae
While lying on your back, gently pulling one knee to your chest can provide relief. If you suffer from spinal stenosis, this flexion-based movement can widen the spinal canal temporarily, offering immediate neurological relief.
Cat-Cow: Mobilizing the Spine Without Stress
The Cat-Cow sequence is the gold standard for restoring mobility. This rhythmic movement helps the small stabilizing muscles of the spine work together, promoting smooth movement without the intensity of heavy weight exercises.
The Chemistry of a Cramp: The Role of Magnesium, Potassium, and Calcium
Magnesium is very important; it works as a natural muscle relaxant at the cellular level and stops the long contractions that cause back spasms. Electrolyte imbalance or nutrient deficiencies can trigger these painful events.
Hydration as a Remedy: Why Dehydration Leads to Nerve Irritation
Dehydration makes your nervous system more sensitive, causing your muscles to overreact to small stresses. Proper water intake is essential to maintain the volume of the spinal disc and prevent nerve compression.
Quick Fixes: Foods and Supplements to Reset Muscle Function
Increase your intake of potassium-rich foods and magnesium-rich sources. If spasms are severe, a magnesium glycinate supplement may help restore systemic balance and support the healing of muscular injury.
Finding the Trigger Point: How to Safely Use a Massage Ball
Use a massage ball against a wall to apply sustained pressure to tender tissue. Do not roll over bony protrusions; focus on the soft tissue beside the spine.
Foam Rolling Techniques for the Upper Back and Rhomboid Muscles
Foam rollers help mobilize the thoracic spine and the rhomboid muscles. This releases tension from poor posture. Avoid using them on the lumbar spine, which lacks the rib cage's protection.
Precautions: Areas to Avoid During an Acute Spasm
If you have a history of degenerative disc disease or facet joint osteoarthritis, be cautious with deep tissue pressure. If you feel sharp, radiating pain, stop immediately, as this may indicate an injury requiring physical therapy.
NSAIDs vs. Acetaminophen: Reducing Inflammation vs. Blocking Pain
Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen are the first defense. They reduce the inflammation that makes pain worse. Acetaminophen targets pain perception but does not treat inflammation.
The Role of Muscle Relaxants and Topical Ointments
If a doctor prescribes muscle relaxants, know that these drugs are short-term tools to break the cycle of acute spasms, allowing you to start basic physical therapy. They are not a long-term solution.
Understanding When Medication is a Tool, Not a Cure
If you only use medication without fixing movement patterns or lifestyle, spasms will likely return once the drugs' effects end. Medication should be a bridge to a spine conditioning program.
The Mind-Body Connection: How Stress Keeps Muscles Contracted
Pain creates a stress response, keeping your sympathetic nervous system on "high alert." Chronic stress ensures your muscles stay guarded and tight.
Deep Diaphragmatic Breathing: Signaling the Back Muscles to Let Go
Taking deep breaths into the belly sends a signal to your brain that you are safe, forcing your body to lower its baseline muscular tension.
The 4-7-8 Technique to Calm the Autonomic Nervous System
The 4-7-8 technique forces the nervous system to decelerate, often proving more effective than aggressive stretching at releasing a stubborn knot.
The Postural Reset: Correcting Position to Unload the Spine
Poor posture is the structural root of most recurrent spasms. Ensure your monitor is at eye level and use an ergonomic chair. Every hour, perform a "postural reset" by pulling your shoulder blades back. This prevents muscle weakness and protects your spine.
Conclusion
Getting relief from Back Spasms requires a multifaceted approach. By integrating thermal therapy, movement, and mindfulness, you regain control over your body’s protective responses. If you experience bladder or bowel control issues, progressive muscle weakness, or sudden numbness, seek emergency care immediately, as these are signs of serious nerve compression. For long-term relief, consult a physical therapist to develop a personalized exercise program. By following these evidence-based home treatment strategies, you can transition from acute pain to a resilient, healthy back.